Consumer Real-Time Pharmacy Benefit Check FHIR IG, published by HL7 International / Pharmacy. This guide is not an authorized publication; it is the continuous build for version 2.0.0-ballot built by the FHIR (HL7® FHIR® Standard) CI Build. This version is based on the current content of https://github.com/HL7/carin-rtpbc/ and changes regularly. See the Directory of published versions
| Page standards status: Informative |
This section has be adjusted. Modifications are italicized.
The goals of the consumer-focused real-time pharmacy benefit check (consumer RTPBC) are:
The real-time pharmacy benefit check is designed to provide accurate cost information based on the specifics of a patient prescription. Details such as the specific drug name, dose form, strength and quantity must match the prescription exactly in order to receive reliable results.
However, a patient may wish to use the process for a medication they haven't yet been prescribed, for example to understand its cost compared to their current treatment. In that circumstance, the results must be viewed as approximate information that may not reflect their actual cost when their prescriber has ordered a particular product and dosage
The previous version's Use Case Flows section and Related Information Flows section have been combined and reworked below.
The patient uses a consumer-facing client application to retrieve and view information related to their medications from their insurer, drug discount sources or other related data sources, as illustrated below.
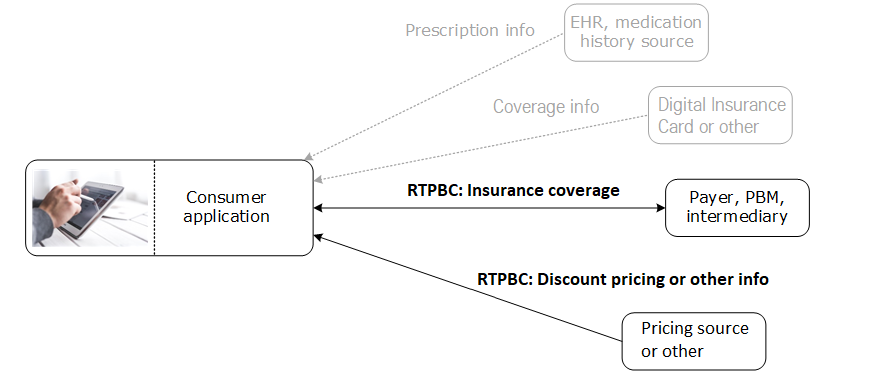
Related information flows outside of consumer RTPBC The patient's app might gather related information (e.g., medication information or insurance eligibility) before submitting the consumer RTPBC request.
The patient learns how how their medication will be covered by their insurance, including out of pocket costs and any coverage restrictions or requirements that might apply

The patient discovers discount pricing or other related information available for their medication.

New in this version
Retrieving member-specific information from an insurer requires use of the full RTPBC request containing protected health information (PHI) such as patient demographics and insurance details which enable the insurer to locate the specific member coverage on which to base its response.
However, when requesting non-patient-specific information such as cash pricing, the Non-PHI RTPBC request may be used.
The actors in RTPBC use cases include:
This section has be adjusted. Modifications are italicized.
This section has be adjusted. Modifications are italicized.
New in this version
The Digital Insurance Card provides standardized insurance identifiers required for CARIN Real-Time Pharmacy Benefit Check (RTPBC) transactions. These identifiers are required in order for consumers to perform real-time pharmacy benefit checks in applications of their choosing, as specified in the CARIN RTPBC Implementation Guide.
A consumer wants to check their pharmacy benefit coverage and medication costs before filling a prescription. The digital insurance card provides the necessary identifiers (member ID, group number, BIN/IIN/PCN) required to submit an RTPBC request through either direct FHIR API access. Consumer application requests access to retrieve the required identifiers from the digital insurance card and upon being granted access by the member, includes those identifiers in an RTPBC request.